A uni- and multivariable quasi-Poisson regression model was used to assess the relationship of the MELD categories with LOS and the number of comorbidities. 
The model was tested for interactions in an exploratory manner and model assumptions were controlled using residual-based methods. 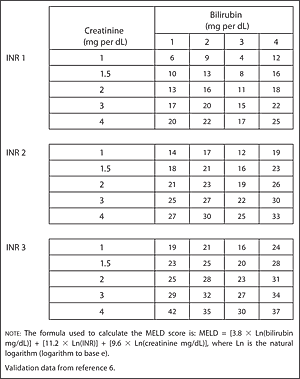
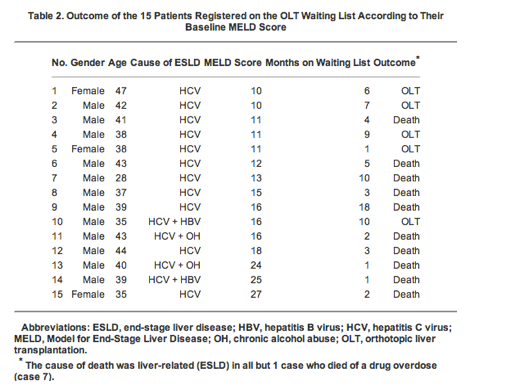
The association of the specific MELD categories with in-hospital mortality was assessed by means of a uni- and multivariable Cox proportional-hazards regression model. The primary and secondary outcome measures were stratified by the MELD score on hospital admission using the following MELD categories: scores of <15, 15 to 19, 20 to 29, and ≥30 points. We therefore aimed to investigate a potential association of the MELD score with mortality, length of hospital stay (LOS), and disease burden in a general patient population. Today, the MELD score is primarily being used to allocate organs for liver transplantation, but recent studies have indicated that the MELD score might be used as a general prognostic tool in patients, independent of the presence of liver disease. Interestingly, the etiology of liver disease was not found to be a relevant predictor of mortality. Subsequently, the MELD score was thoroughly validated in patients with a broad spectrum of liver diseases showing an excellent discriminatory power for prediction of short-term mortality. It has been developed and validated to predict mortality in patients with portal hypertension undergoing placement of transjugular intrahepatic portosystemic shunts. The well-established MELD score depends on 3 readily available laboratory variables, that is, serum creatinine, serum bilirubin, and the international normalized ratio (INR). The laboratory-based model for end-stage liver disease (MELD) score reflects the function of the kidney, liver, and extrinsic coagulation pathway and might be used as a general prognostic tool for the assessment of patients. We suggest to prospectively validate the MELD score in inpatients as part of clinical decision support systems.Ĭlinical decision support systems have been shown to improve the quality of patient care and to reduce health care costs however, little is known about their overall impact on patient outcomes. In our study population consisting of adult inpatients, the MELD score on hospital admission was significantly associated with mortality, LOS, and the number of comorbidities. Increased MELD scores of 15 to 19, 20 to 29, and ≥30 points were positively associated with LOS and the number of comorbidities in uni- and multivariable analysis. The primary outcome measure was in-hospital all-cause mortality secondary outcome measures were LOS and the number of comorbidities.Ī total of 39,323 inpatients were included in the final analysis. The MELD score on hospital admission was calculated retrospectively. From January 2012 through December 2013, all consecutive inpatients aged 18 years were eligible for the study patients with missing MELD parameters on hospital admission and/or treatments influencing the international normalized ratio, that is, novel oral anticoagulants and vitamin K antagonists, were excluded. We performed a retrospective observational study at a tertiary referral center.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
